Interventional Pain Management at Niramaya Spine Care
Chronic back and neck pain can affect every part of life — movement, work, sleep, and even mental well-being. Managing this pain early and effectively helps prevent long-term disability, mood disturbances, and reduced quality of life.
Interventional pain management offers a science-based alternative to long-term medication use or major surgery. These minimally invasive, image-guided procedures directly target the source of pain, helping reduce inflammation, calm irritated nerves, and restore mobility.
At Niramaya Spine Care, our specialists are trained in a wide spectrum of interventional techniques. Treatments are performed with fluoroscopic or ultrasound guidance to ensure precision and safety.
Whether you’re experiencing chronic or acute spine-related pain, we provide individualized treatment plans focused on improving function and enhancing day-to-day comfort. Our aim is simple:
to relieve pain ethically and restore meaningful movement in your life.
📌 Benefits of Interventional Pain Management
- Minimally invasive, targeted treatment
- Avoids long-term pain medication side effects
- Reduces the need for major surgery
- Improves mobility and function
- Performed under precise imaging guidance
Types of Interventional Pain Management Treatments
At Niramaya Spine Care, interventional pain procedures are selected based on the pain generator, underlying pathology, and the level of functional limitation. Our approach begins with least invasive techniques, progressing only when necessary.
🎯 Targeted Pain Relief Treatments
These procedures precisely address the source of pain using image-guided injections.
- Nerve Blocks: Blocks pain signals from irritated nerves (e.g., sciatica, chronic neck pain).
- Joint Injections: Targets inflammation in spinal joints such as facet joints or sacroiliac joints.
- Epidural Steroid Injections: Reduces nerve inflammation caused by disc herniation, stenosis, or nerve compression.
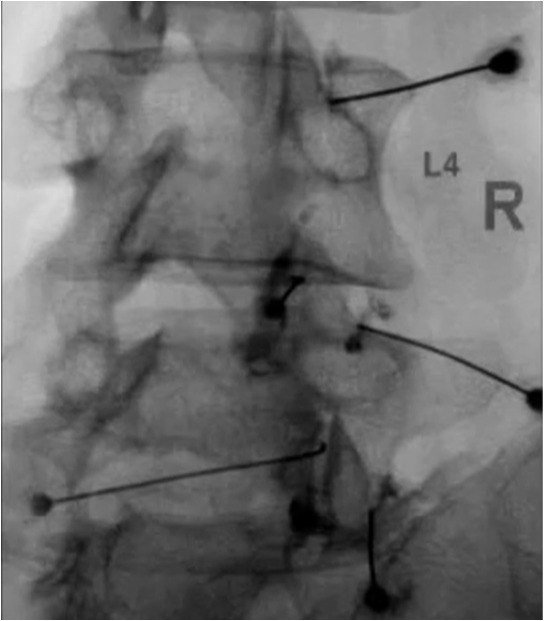
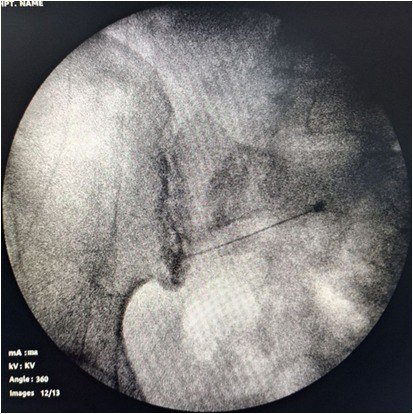
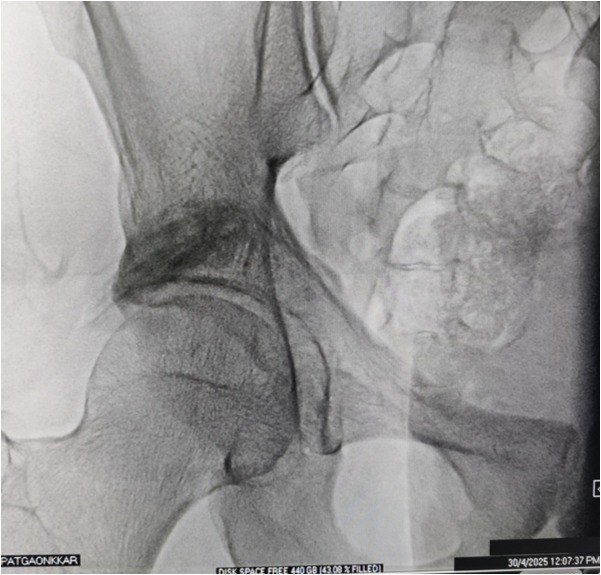
🧬 Advanced Image-Guided Procedures
Used when pain is persistent or associated with structural abnormalities.
- Radiofrequency Ablation (RFA): Uses heat to silence pain-causing nerves, commonly for facet joint and SI joint pain.
⚡ Life-Changing Interventions for Complex Pain
Reserved for patients with severe, chronic, or refractory pain where conservative and advanced injections are insufficient.
- Peripheral Nerve Stimulation (PNS): Electrical impulses calm overactive pain pathways for chronic nerve pain.
- Intrathecal Drug Delivery (Pain Pump): Medication delivered directly into spinal fluid for severe, long-standing pain.
- Spinal Cord Stimulation (SCS): Electrical modulation of spinal pain signals to relieve chronic back or leg pain.
🌿 Tailored to Every Patient
Every procedure is recommended only when scientifically indicated, supported by:
- Clinical examination
- MRI/X-ray correlation
- Pain pattern mapping
- Function-focused recovery goals
📌 The aim is not just to reduce pain—but to restore meaningful movement and quality of life
Benefits of Interventional Pain Management
Interventional pain techniques are designed to treat the root cause of pain, not just mask symptoms.
- Minimally invasive alternatives to surgery: These procedures use tiny needles or probes, avoiding large incisions and faster return to activities.
- Direct, targeted pain relief: Pain sources such as nerves, joints or compressed tissues are treated precisely using image-guided injections or ablation.
- Reduced need for long-term medications: Helps avoid the side effects of painkillers, such as acidity, constipation, dependency, or drowsiness.
- Improves mobility and function: By calming inflamed or irritated nerves, patients regain movement, posture, sleep quality, and activity levels.
- Safe and scientifically guided: Fluoroscopy or ultrasound ensures accuracy, minimizing risk and enhancing success rates.

Goal: Not just pain reduction, but improved function, activity, and quality of life
Before the Procedure
A detailed evaluation is essential to ensure that the treatment targets the correct pain generator.
- Clinical examination & history: Your doctor studies movement limitations, pain pattern, and nerve involvement.
- Review of Investigations: MRI, X-ray, CT, or nerve studies help confirm the exact anatomical cause of pain.
- Eligibility & medical condition review: Diabetes, blood thinners, osteoporosis, infections, allergies, and prior spine procedures are assessed.
- Planning the right procedure: Based on diagnosis, the most suitable intervention (e.g., nerve block, epidural, RFA, SIJ injection) is selected.
Pre-procedure instructions
- Fasting if sedation is required
- Adjustment of blood thinners/ stop blood thinners 5 days prior to procedure
- Arrive with a relative for support
- Light meal restrictions (varies per procedure)
Purpose: Ensure the treatment is appropriate, safe, and likely to give meaningful results.
During the Procedure
Most procedures are day-care, meaning no hospital admission is usually needed.
- Positioning & sterilization: The area is cleaned thoroughly and positioned correctly to access the target safely.
- Local anesthesia or light sedation: Ensures comfort; patients typically feel pressure but not pain.
- Imaging-guided targeting: Fluoroscopy or ultrasound helps the doctor visualize the exact structure causing pain.
- Precise treatment delivery: Medication to reduce inflammation,Heat energy for nerve ablation (RFA), Electrical stimulation (nerve modulation)
- Short procedure time: Generally 15 to 45 minutes, depending on complexity.
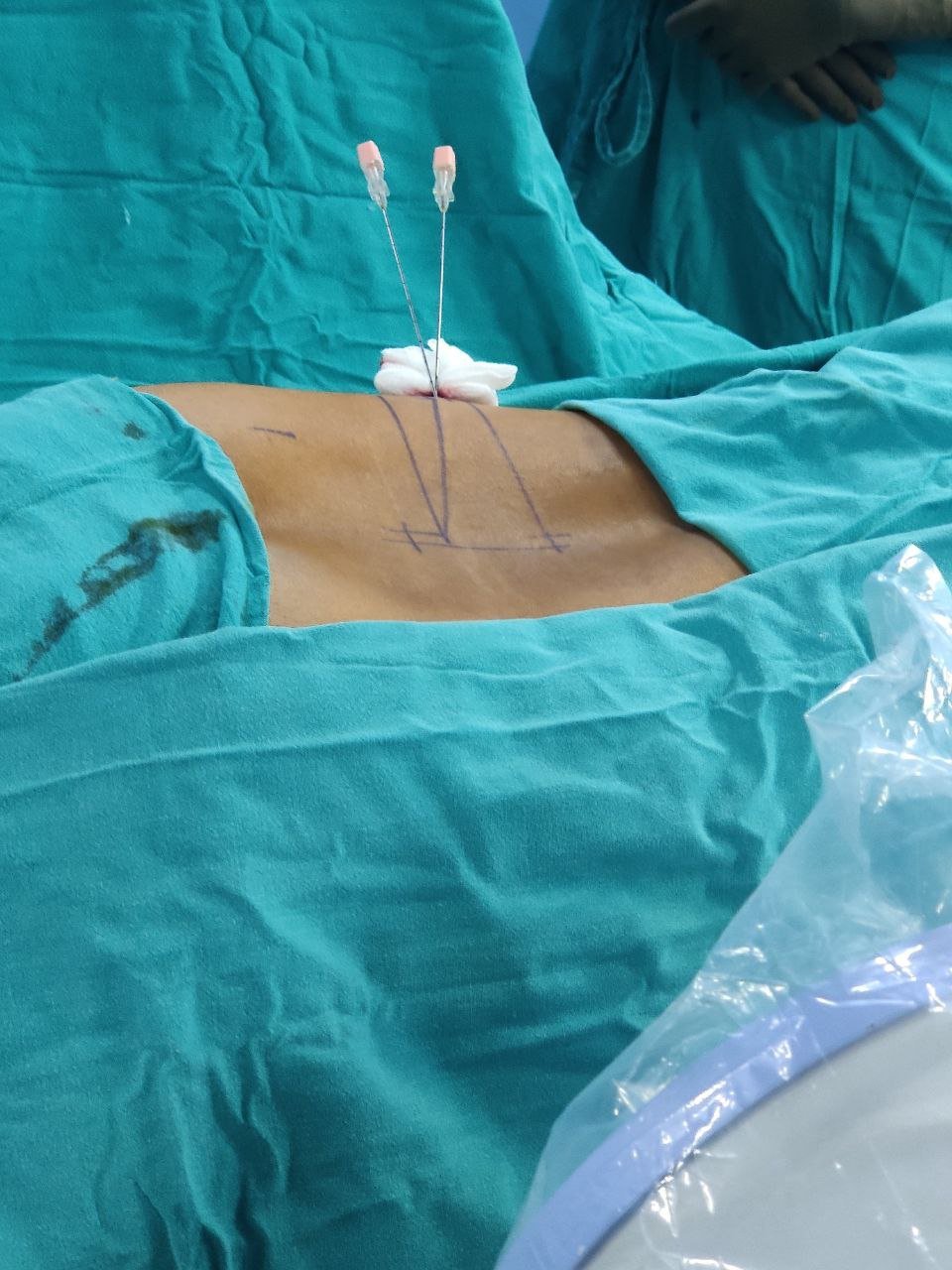
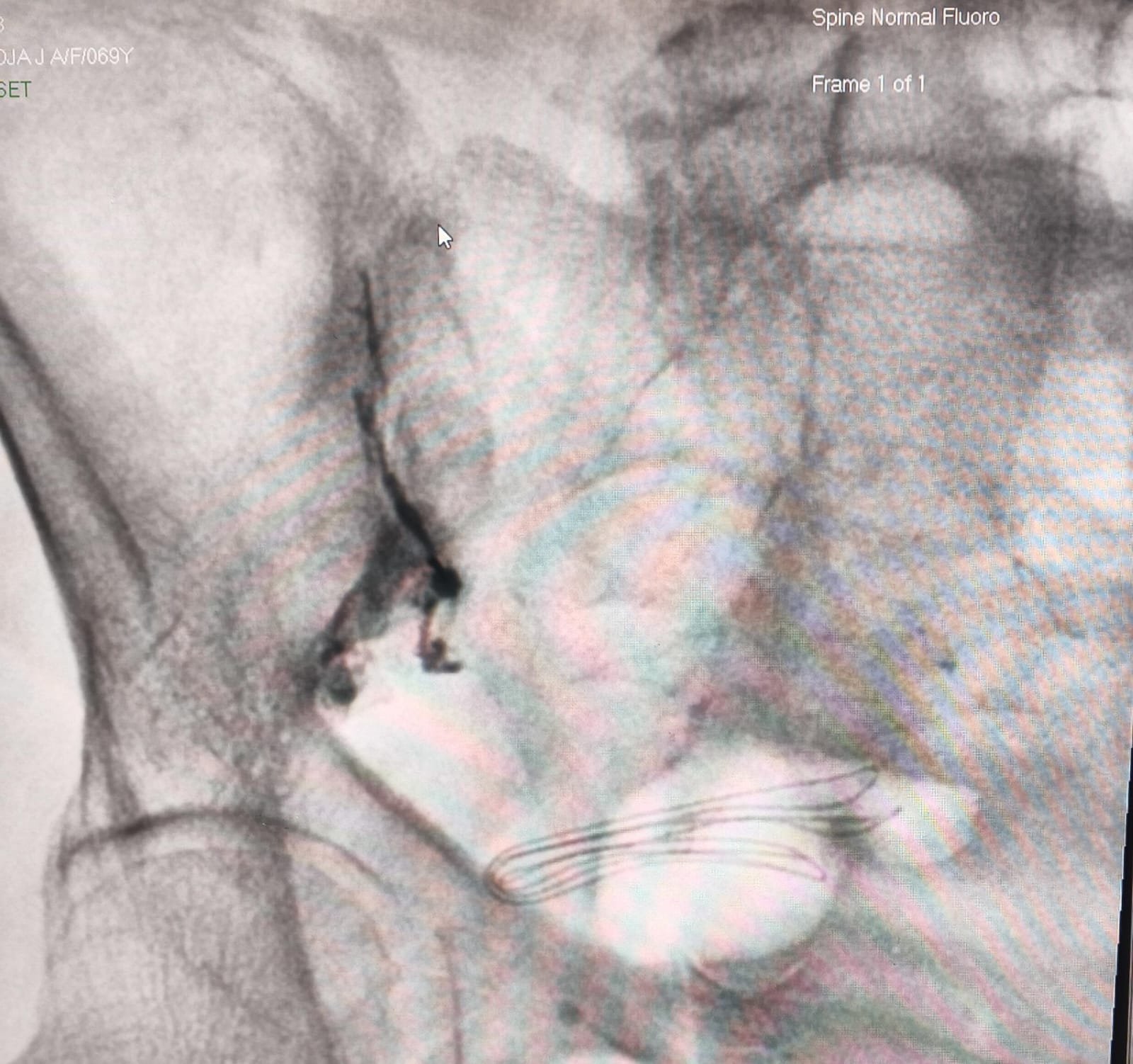
Experience: Most patients tolerate the procedure well, with minimal discomfort.
After the Procedure
Recovery is usually quick as these are minimally invasive treatments.
- Short observation period: Patients are monitored briefly for comfort and vitals before discharge.
- Relief pattern varies: Some feel instant relief, while others improve gradually over days as inflammation settles
Post-procedure instructions:
- Avoid heavy lifting for 2–5 days
- Resume home/office activities gradually
- Continue prescribed exercises or physiotherapy
- Maintain correct posture and ergonomics


- Follow-up & monitoring: Pain relief, functional improvement, medication needs, and further sessions are reviewed.
- Long-term focus: Treatment is combined with physiotherapy, strengthening and posture correction to ensure durability of results.
Outcome Goal: Long-term mobility, reduced pain episodes, and improved day-to-day functioning.
