Understanding Spinal Infections
Spinal infections are serious conditions caused by bacteria, tuberculosis, fungi, or other microorganisms that affect the bones, discs, or surrounding structures of the spine. If not diagnosed and treated early, they can lead to severe pain, spinal instability, nerve damage, or even paralysis. Prompt medical evaluation and timely treatment are essential for a good outcome.
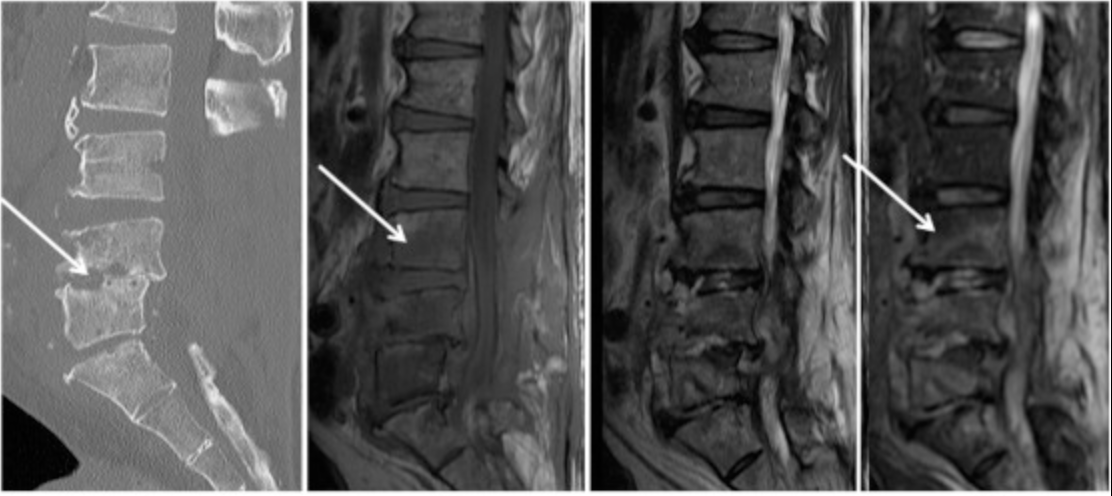
Types of Spinal Infections
1. Vertebral Osteomyelitis
Infection of the vertebral bones, often spreading through the bloodstream from another part of the body.
2. Discitis
Infection of the intervertebral disc space, more common in children but also seen in adults.
3. Spinal Epidural Abscess
Collection of pus around the spinal cord that can compress nerves and requires urgent treatment.
4. Tuberculous Spine (Pott’s Disease)
A common form of spinal infection in developing countries, causing gradual bone destruction, deformity, and neurological deficits.
Common Symptoms
- Persistent back or neck pain not relieved by rest
- Fever, chills, or night sweats
- Unexplained weight loss
- Localized spinal tenderness
- Difficulty walking or limb weakness
- Numbness, tingling, or bowel/bladder disturbances (in advanced cases)
Causes and Risk Factors
- Bloodstream infections
- Diabetes or poor immunity
- Recent spine surgery or injections
- Tuberculosis exposure
- Intravenous drug use
- Long-term steroid use
- Chronic kidney disease
Diagnosis
Accurate diagnosis is crucial and may include:
- Blood tests (ESR, CRP, blood cultures)
- MRI spine (gold standard for early detection)
- CT scan for bone involvement
- Biopsy or aspiration to identify the causative organism
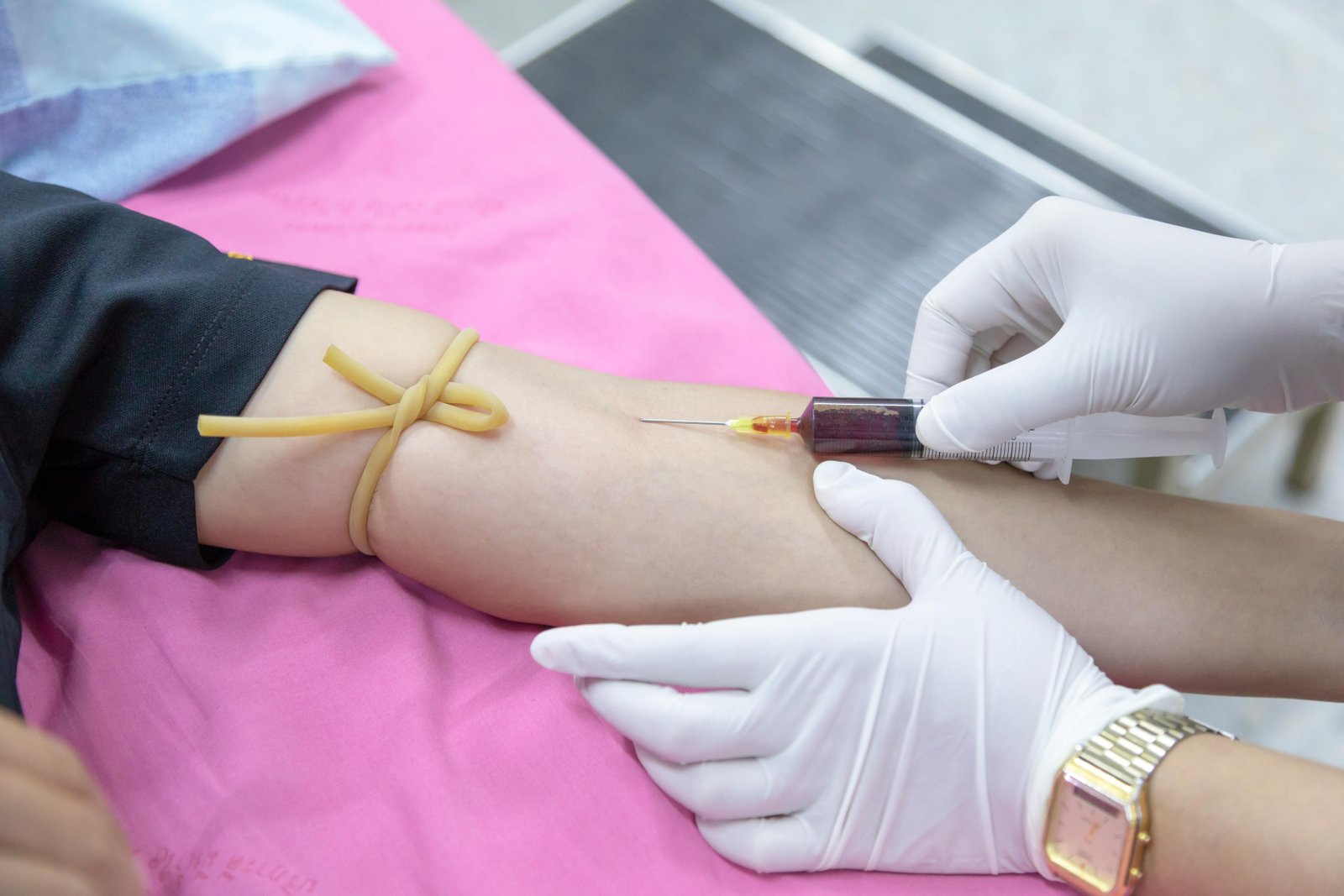

Treatment Options
Conservative (Non-Surgical) Treatment
- Targeted intravenous or oral antibiotics
- Anti-tubercular therapy (for TB spine)
- Pain control and spinal support
- Close clinical and radiological monitoring
Surgical Treatment (When Required)
Surgery may be needed in cases of:
- Neurological deficits
- Spinal instability or deformity
- Failure of medical treatment
- Large abscess causing compression
- Decompression of nerves
- Drainage of abscess
- Stabilization of the spine
- Prevention of permanent neurological damage
🔹 Endoscopic Spine Surgery for Infections (Minimally Invasive)
Endoscopic surgery allows targeted removal of infected tissue with minimal damage to normal structures.
Advantages:
- Small incision
- Minimal muscle damage
- Effective drainage of abscess
- Faster recovery
- Reduced blood loss
- Ideal for selected cases of discitis and epidural abscess
Common Procedures:
- Endoscopic debridement and drainage
- Endoscopic discectomy for infected discs
- Targeted biopsy and decompression
🔹 Open Spine Surgery for Infections
Indications:
- Severe spinal instability
- Large bony destruction
- Significant deformity
- Multi-level involvement
- Failed minimally invasive approach
Procedures may include:
- Open decompression
- Extensive debridement
- Abscess drainage
- Instrumentation and fusion for stability
Recovery and Follow-Up
- Long-term antibiotics or anti-TB therapy (6–12 months in TB)
- Gradual mobilization with physiotherapy
- Regular clinical, laboratory, and radiological follow-up
- Focus on nutrition and immune health
Key Message for Patients
Early diagnosis and appropriate treatment are critical in spinal infections. With modern imaging, targeted antibiotics, and advanced surgical techniques—including endoscopic minimally invasive spine surgery—excellent outcomes are achievable in most patients.
