When One Vertebra Slips Forward Over Another
What is Spondylolisthesis?
Spondylolisthesis is a spinal condition in which one vertebra slips forward over the vertebra below it, most commonly in the lower (lumbar) spine. This slippage can lead to back pain, leg pain, nerve compression, and spinal instability, affecting daily activities and quality of life.
The condition may develop gradually or appear after injury, and its severity can range from mild and asymptomatic to severe with neurological symptoms.
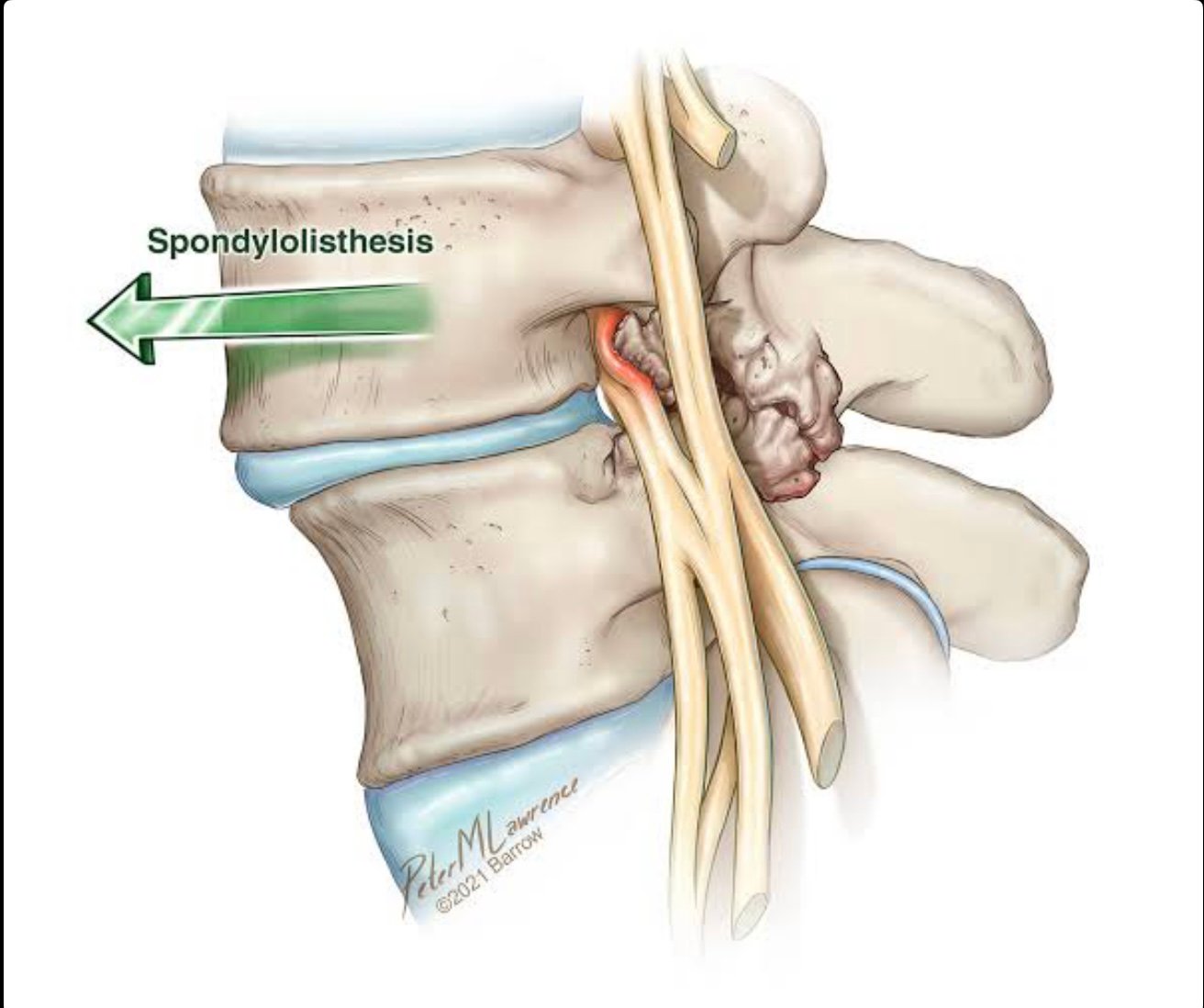
What Happens in Spondylolisthesis?
In a healthy spine, vertebrae are stacked and aligned. In spondylolisthesis, this alignment is disturbed due to:
- Defects in the vertebra
- Degenerative changes
- Stress fractures
- Trauma or congenital weakness
This forward slip can narrow the spinal canal or nerve exit pathways, leading to pain, numbness, or weakness in the legs.
Types of Spondylolisthesis
- Isthmic – Due to a defect or stress fracture in the pars interarticularis (common in younger patients)
- Degenerative – Due to age-related disc and joint degeneration (common in older adults)
- Congenital – Present from birth due to abnormal spinal development
- Traumatic – Caused by acute injury
- Pathological – Due to bone disease, infection, or tumors
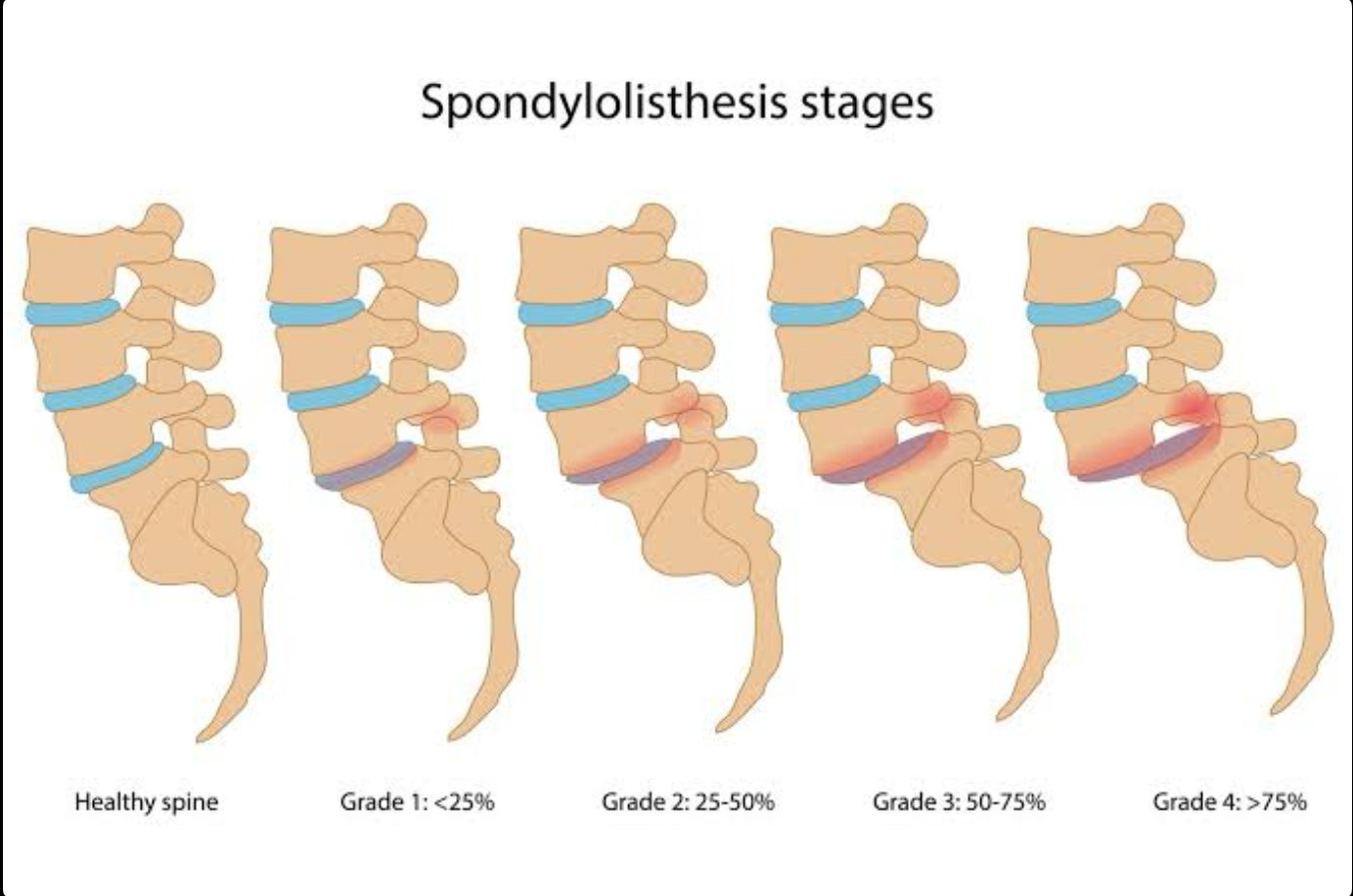
Stages (Grades) of Spondylolisthesis
Spondylolisthesis is graded based on the percentage of vertebral slippage:
🔹 Grade I (Mild)
- < 25% slip
- Often asymptomatic or mild back pain
- Usually managed conservatively
🔹 Grade II (Moderate)
- 25–50% slip
- Back pain with possible leg pain
- May require injections or advanced physiotherapy
🔹 Grade III (Severe)
- 50–75% slip
- Significant pain, posture changes, nerve symptoms
- Surgical evaluation often required
🔹 Grade IV (Very Severe)
- 75–100% slip
- Marked instability and neurological compromise
- Surgery is usually necessary
🔹 Grade V (Spondyloptosis)
- Complete vertebral displacement
- Rare and severe condition
- Requires complex surgical correction
Common Symptoms
- Persistent lower back pain
- Pain radiating to buttocks or legs
- Tight hamstrings
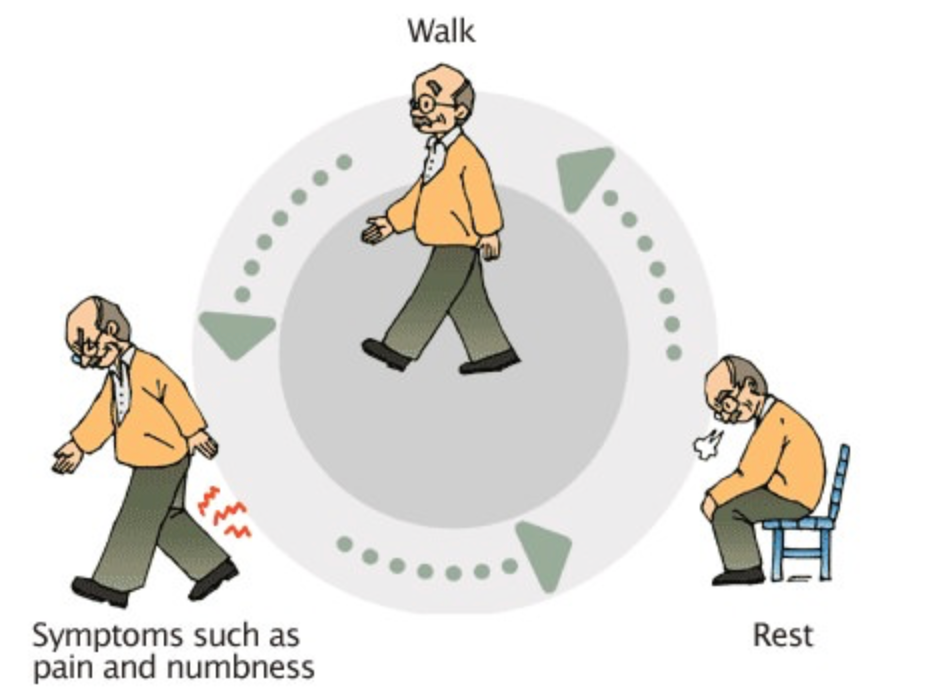
- Numbness or tingling in legs
- Difficulty standing or walking for long periods
- Postural changes in advanced stages
Diagnosis
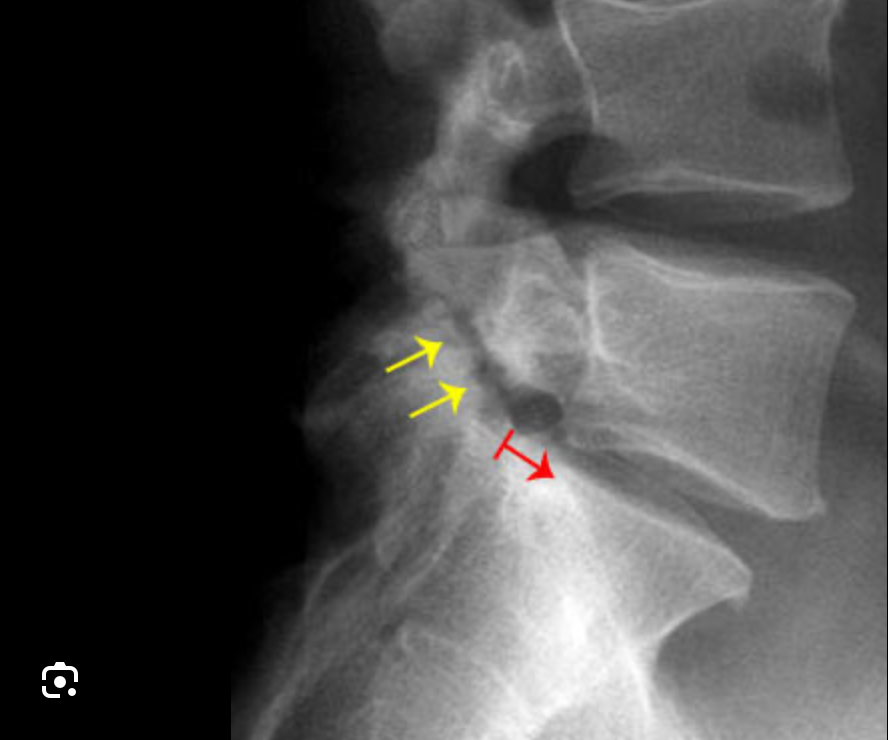
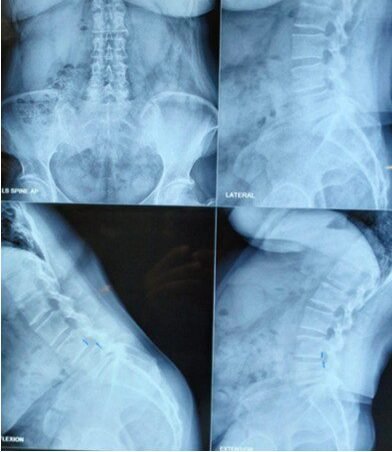
- X-rays (standing lateral views) to assess slippage
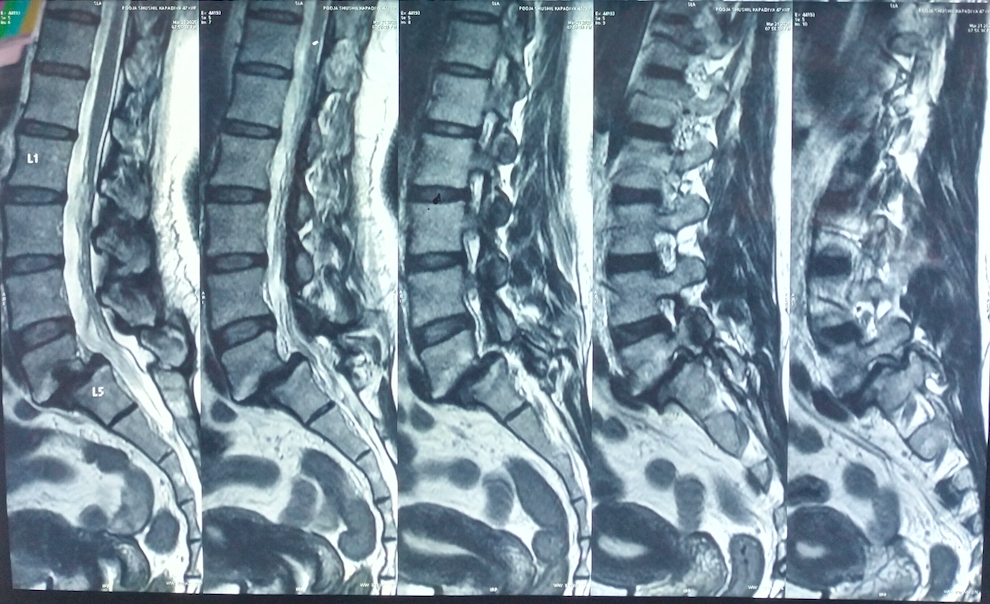
- MRI to evaluate nerve compression and discs
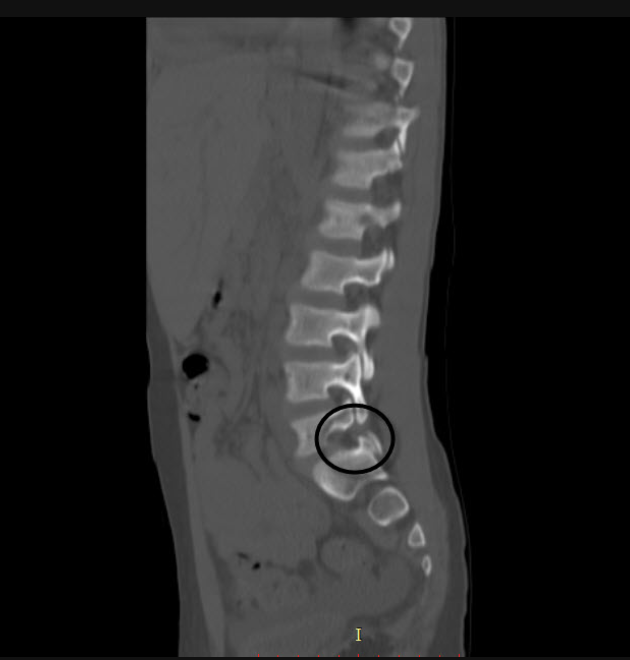
- CT scan for bony defects (especially pars defects)
- Dynamic X-rays to assess instability
Treatment
Conservative (First-line for early stages)
- Activity modification
- Physiotherapy and core strengthening
- Pain medications
- Bracing (selected cases)
- Image-guided spinal injections

Surgical Treatment (For advanced or symptomatic cases)
- Decompression of nerves
- Spinal stabilization and fusion
- Minimally Invasive Spine Surgery (MISS) or Endoscopic techniques where appropriate
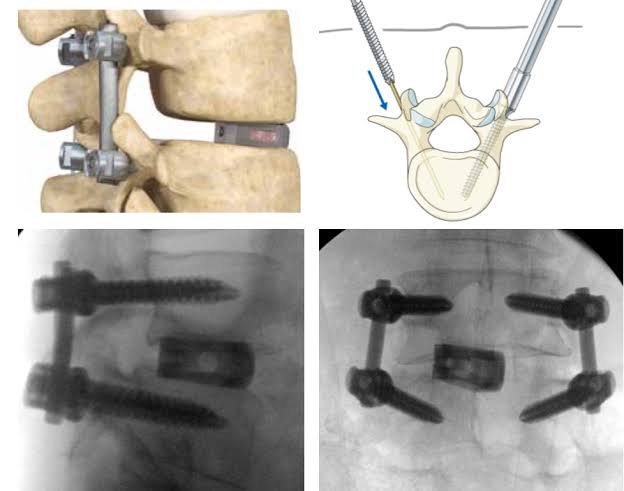
The choice of treatment depends on grade, symptoms, instability, and patient lifestyle.
When Should You See a Spine Specialist?
- Pain persisting despite conservative care
- Progressive leg pain or weakness
- Difficulty walking or standing
- Evidence of worsening slip on imaging
